Herpesvirus infections and immunological disturbances in patients with different stages of Alzheimer’s disease
- Authors: Krynskiy S.A.1, Malashenkova I.K.1,2, Ogurtsov D.P.1,2, Khailov N.A.1, Chekulaeva E.I.1, Shipulina O.Y.3, Ponomareva E.V.4, Gavrilova S.I.4, Didkovsky N.A.2, Velichkovsky B.M.1
-
Affiliations:
- NRC «Kurchatov Institute»
- FSBI «Federal Scientific and Clinical Center for Physico-Chemical Medicine of the Federal Medical and Biological Agency»
- FSBI «Central Research Institute for Epidemiology» of the Federal Service for Surveillance of Consumer Rights Protection and Human Wellbeing (Rospotrebnadzor)
- FSBSI «Mental Health Research Center»
- Issue: Vol 66, No 2 (2021)
- Pages: 129-139
- Section: ORIGINAL RESEARCHES
- URL: https://journals.rcsi.science/0507-4088/article/view/118157
- DOI: https://doi.org/10.36233/0507-4088-32
- ID: 118157
Cite item
Abstract
Introduction. Alzheimer’s disease (AD) is a multifactorial disease that leads to a progressive memory loss, visualspatial impairments, emotional and personality changes. As its earliest pre-dementia clinical stage, amnestic mild cognitive impairment syndrome (aMCI) is currently considered. Neuroinflammation plays a role in the development and progression of aMCI and the initial stage of AD, which can be supported by immunological disorders of a systemic character. Study of factors, including infections, influencing immune disorders and systemic inflammatory response in patients with aMCI, is of great importance.
The aim of this study was to obtain new data on the possible role of herpesvirus infections in the development and progression of aMCI.
Material and methods. 100 patients with aMCI diagnosis, 45 patients with AD, 40 people from the control group were enrolled into the study. The frequency of DNA detection of herpesviruses (Epstein–Barr virus (EBV), human herpesviruses (HHV) type 6 and 7, cytomegalovirus (CMV)), the levels of viral load and the serological markers of herpesvirus infections (IgG to HHV-1, IgG to CMV) were determined. Immunological studies included an assessment of the level of the main pro-inflammatory and anti-inflammatory cytokines, and indicators of humoral and cellular immunity.
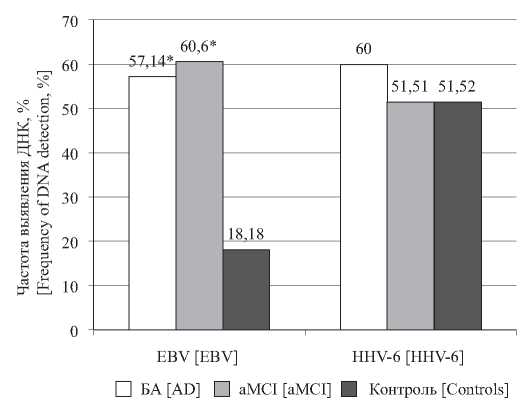
Results. The study found an increased detection rate of EBV in saliva and a higher level of EBV DNA in saliva in aMCI and AD than in the control group. A relationship between the presence of active EBV infection and changes in immunological parameters in patients with aMCI were found. It was also discovered that the level of IgG antibodies to CMV is associated with the stage of AD.
Discussion. The results indicate a possible role of EBV- and CMV-induced infections in the development of immunological changes which are typical for mild cognitive impairment and in the progression of AD.
Conclusion. The obtained data can be important for prognostic methods addressing AD development, including its pre-dementia stage, and for new approaches to individualized treatment and prevention.
Full Text
##article.viewOnOriginalSite##About the authors
S. A. Krynskiy
NRC «Kurchatov Institute»
Author for correspondence.
Email: srgkr002@gmail.com
ORCID iD: 0000-0003-4328-865X
Krynskiy Sergey Andreevich, Ph.D. (Med.), researcher. SPIN: 4465-0413
123182, Moscow
+7(499)1969539
I. K. Malashenkova
NRC «Kurchatov Institute»; FSBI «Federal Scientific and Clinical Center for Physico-Chemical Medicine of the Federal Medical and Biological Agency»
Email: malashenkova.irina@bk.ru
ORCID iD: 0000-0002-3604-9098
Malashenkova Irina Konstantinovna, Ph.D. (Med.), head of the laboratory of molecular immunology and virology. SPIN: 4205-6010
123182, Moscow
119435, Moscow
8(916)935-73-09
D. P. Ogurtsov
NRC «Kurchatov Institute»; FSBI «Federal Scientific and Clinical Center for Physico-Chemical Medicine of the Federal Medical and Biological Agency»
Email: ogurtsovdp@gmail.com
ORCID iD: 0000-0003-0257-4713
Ogurtsov Daniil Pavlovich, Ph.D. (Med.), researcher. SPIN: 7288-1161
123182, Moscow
119435, Moscow
+7(499)1969539
N. A. Khailov
NRC «Kurchatov Institute»
Email: nik_khailov@bk.ru
ORCID iD: 0000-0002-3693-285X
Khailov Nikita Anatolievich, Ph.D. (Med.), senior researcher. SPIN: 7926-9505
123182, Moscow
+7(499)1969539
E. I. Chekulaeva
NRC «Kurchatov Institute»
Email: chekulaevakatarina@gmail.com
ORCID iD: 0000-0002-2559-2132
Chekulaeva Ekaterina Igorevna, junior researcher
123182, Moscow
+7(499)1969539
O. Y. Shipulina
FSBI «Central Research Institute for Epidemiology» of the Federal Service for Surveillance of Consumer Rights Protection and Human Wellbeing (Rospotrebnadzor)
Email: olga.shipulina@pcr.ru
ORCID iD: 0000-0003-4679-6772
Shipulina Ol’ga Yurievna, Ph.D. (Med.), head of the laboratory of molecular methods of diagnostics. SPIN: 9235-1239
111123, Moscow
+7(495)9749646
E. V. Ponomareva
FSBSI «Mental Health Research Center»
Email: elena-pon@hotmail.com
ORCID iD: 0000-0002-2835-5706
Ponomareva Elena Valerievna, Ph.D. (Med.), senior researcher. SPIN: 3933-6900
115522, Moscow
+7 (495)1090393
S. I. Gavrilova
FSBSI «Mental Health Research Center»
Email: sigavrilova@yandex.ru
ORCID iD: 0000-0001-6683-0240
Gavrilova Svetlana Ivanovna, D.Sci. (Med.), professor, head of the department of geriatric psychiatry. Author ID: 113647
115522, Moscow
+7 (495)1090393
N. A. Didkovsky
FSBI «Federal Scientific and Clinical Center for Physico-Chemical Medicine of the Federal Medical and Biological Agency»
Email: didkovskinic@gmail.com
ORCID iD: 0000-0001-6567-5998
Didkovsky Nikolay Antonovich, D.Sci. (Med.), professor, head of the laboratory of clinical immunology. SPIN: 6146-5134
119435, Moscow
+7(499)2467721
B. M. Velichkovsky
NRC «Kurchatov Institute»
Email: Boris.Velichkovsky@tu-dresden.de
ORCID iD: 0000-0001-7823-0605
Velichkovsky Boris Mitrofanovich, D.Sci. (Psychol.), professor, head researcher
123182, Moscow
+7(499)1969539
References
- Manly J.J, Tang M., Schupf N., Stern Y., Vonsattel J.G., Mayeux R. Frequency and course of mild cognitive impairment in a multiethnic community. Ann. Neurol. 2008; 63(4): 494–506. https://doi.org/10.1002/ana.21326.
- Alzheimer’s Disease International. World Alzheimer Report 2018. The State of the Art of Dementia Research: New Frontiers. London: Alzheimer’s Disease International (ADI); 2018. Available at: https://www.alz.co.uk/research/WorldAlzheimerReport2018.pdf (accessed March 22, 2021).
- Малашенкова И.К., Крынский С.А., Хайлов Н.А., Огурцов Д.П., Пономарёва Е.В., Гаврилова С.И., и др. Адаптивный иммунитет, системное воспаление и уровень основных цитокинов у пациентов с болезнью Альцгеймера различных стадий и мягким когнитивным снижением амнестического типа. Аллергология и иммунология. 2018; 19(4): 206–14.
- Малашенкова И.К., Крынский С.А., Хайлов Н.А., Огурцов Д.П., Селезнева Н.Д., Фёдорова Я.Б., и др. Противовоспалительные эффекты нейротрофической терапии (применение церебролизина при мягком когнитивном снижении). Журнал неврологии и психиатрии им. С.С. Корсакова. 2018; 118(5): 39–44. https://doi.org/10.17116/jnevro20181185139.
- Симонов А.Н., Клюшник Т.П., Андросова Л.В., Михайлова Н.М. Использование кластерного анализа и логистической регрессии для оценки риска болезни Альцгеймера у пациентов с синдромом мягкого когнитивного снижения амнестического типа. Журнал неврологии и психиатрии им. C.C. Корсакова. 2018; 118(12): 40–3. https://doi.org/10.17116/jnevro201811812140.
- Carbone I., Lazzarotto T., Ianni M., Porcellini E., Forti P., Masliah E., et al. Herpes virus in Alzheimer’s disease: relation to progression of the disease. Neurobiol. Aging. 2014; 35(1): 122–9. https://doi.org/10.1016/j.neurobiolaging.2013.06.024.
- Letenneur L., Pérès K., Fleury H., Garrigue I., Barberger-Gateau P., Helmer C., et al. Seropositivity to herpes simplex virus antibodies and risk of Alzheimer’s disease: a population-based cohort study. PLoS One. 2008; 3(11): e3637. https://doi.org/10.1371/journal.pone.0003637.
- Blasko I., Knaus G., Weiss E., Kemmler G., Winkler C., Falkensammer G., et al. Cognitive deterioration in Alzheimer’s disease is accompanied by increase of plasma neopterin. J. Psychiatr. Res. 2007; 41(8): 694–701. https://doi.org/10.1016/j.jpsychires.2006.02.001.
- Stein P.S., Steffen M.J., Smith C., Jicha G., Ebersole J.L., Dolph D. Serum antibodies to periodontal pathogens are a risk factor for Alzheimer’s disease. Alzheimer’s Dement. 2012; 8(3): 196–203. https://doi.org/10.1016/j.jalz.2011.04.006.
- Kamer A.R., Craiga R.G., Pirraglia E., Dasanayake A.P., Norman R.G., Boylan R.J., et al. TNF-α and antibodies to periodontal bacteria discriminate between Alzheimer’s disease patients and normal subjects. J. Neuroimmunol. 2009; 216(1–2): 92–7. https://doi.org/10.1016/j.jneuroim.2009.08.013.
- Didkovskii N.A., Malashenkova I.K., Tanasova A.N., Zuikov I.A., Zuikova I.N., Khitrik N.M., et al. Pathogenetic aspects of severe course of herpetic infection. Bull. Exp. Biol. Med. 2007; 2(76): 76–81. https://doi.org/10.1007/s10517-007-0349-7.
- Hemling N., Röyttä M., Rinne J., Pöllänen P., Broberg E., Tapio V., et al. Herpesviruses in brains in Alzheimer’s and Parkinson’s diseases. Ann. Neurol. 2003; 54(2): 267–71. https://doi.org/10.1002/ana.10662.
- Lin W.R., Wozniak M.A., Cooper R.J., Wilcock G.K., Itzhaki R.F. Herpesviruses in brain and Alzheimer’s disease. J. Pathol. 2002; 197(3): 395–402. https://doi.org/10.1002/path.1127.
- Zilka N., Kazmerova Z., Jadhav S., Neradil P., Madari A., Obetkova D., et al. Who fans the flames of Alzheimer’s disease brains? Misfolded tau on the crossroad of neurodegenerative and inflammatory pathways. J. Neuroinflammation. 2012; 9: 47. https://doi.org/10.1186/1742-2094-9-47.
- Kuhla A., Ludwig S.C., Kuhla B., Münch G., Vollmar B. Advanced glycation end products are mitogenic signals and trigger cell cycle reentry of neurons in Alzheimer’s disease brain. Neurobiol. Aging. 2015; 36(2): 753–61. https://doi.org/10.1016/j.neurobiolaging.2014.09.025.
- Doens D., Fernández P.L. Microglia receptors and their implications in the response to amyloid β for Alzheimer’s disease pathogenesis. J. Neuroinflammation. 2014; 11: 48. https://doi.org/10.1186/17422094-11-48.
- Крынский С.А., Малашенкова И.К., Хайлов Н.А., Огурцов Д.П., Чекулаева Е.И., Пономарёва Е.В., и др. Иммунологические маркеры долгосрочных эффектов терапии у пациентов с синдромом мягкого когнитивного снижения. Медицинский академический журнал. 2019; 19(S1): 84–6.
- Дидковский Н.А., Огурцов Д.П., Крынский С.А., Гурская О.Г., Шипулина О.Ю., Домонова Э.А., и др. Миалгический энцефаломиелит/синдром хронической усталости: уровень репликации лимфотропных герпетических вирусов и иммунная защита. Поликлиника. 2016; (5): 46–50.
- Denaro F.J., Staub P., Colmer J., Freed D.M. Coexistence of Alzheimer disease neuropathology with herpes simplex encephalitis. Cell. Mol. Biol. (Noisy-le-Grand). 2003; 49(8): 1233–40.
- Wozniak M.A., Shipley S.J., Combrinck M., Wilcock G.K., Itzhaki R.F. Productive herpes simplex virus in brain of elderly normal subjects and Alzheimer’s disease patients. J. Med. Virol. 2005; 75(2): 300–6. https://doi.org/10.1002/jmv.20271.
- Jamieson G.A., Maitland N.J., Wilcock G.K., Yates C.M., Itzhaki R.F. Herpes simplex virus type 1 DNA is present in specific regions of brain from aged people with and without senile dementia of the Alzheimer type. J. Pathol. 1992; 167(4): 365–8. https://doi.org/10.1002/path.1711670403.
- Honjo K., van Reekum R., Verhoeff N. Alzheimer’s disease and infection: Do infectious agents contribute to progression of Alzheimer’s disease? Alzheimer’s Dement. 2009; 5(4): 348–60. https://doi.org/10.1016/j.jalz.2008.12.001.
- Kobayashi N., Nagata T., Shinagawa S., Oka N., Shimada K., Shimizu A., et al. Increase in the IgG avidity index due to herpes simplex virus type 1 reactivation and its relationship with cognitive function in amnestic mild cognitive impairment and Alzheimer’s disease. Biochem. Biophys. Res. Commun. 2013; 430(3): 907–11. https://doi.org/10.1016/j.bbrc.2012.12.054.
- Lövheim H., Olsson J., Weidung B., Johansson A., Eriksson S., Hallmans G., et al. Interaction between cytomegalovirus and herpes simplex virus type 1 associated with the risk of Alzheimer’s disease development. J. Alzheimers Dis. 2018; 61(3): 939–45. https://doi.org/10.3233/JAD-161305.
Supplementary files