在对炎症性肠病患者进行随访时采用德尔菲法确定一份通过问卷评估的参数清单
- 作者: Shumskaya Y.F.1, Akhmedzyanova D.A.1, Mnatsakanyan M.G.2, Kolosova K.Y.2, Tashchyаn O.V.2, Yurazh M.V.2, Reshetnikov R.V.1
-
隶属关系:
- Research and Practical Clinical Center for Diagnostics and Telemedicine Technologies
- The First Sechenov Moscow State Medical University
- 期: 卷 4, 编号 4 (2023)
- 页面: 481-491
- 栏目: 原创性科研成果
- URL: https://journals.rcsi.science/DD/article/view/262951
- DOI: https://doi.org/10.17816/DD545997
- ID: 262951
如何引用文章
详细
论证。炎症性肠病患者通常需要医生的终生随访。远程随访是提供此类医疗服务的一个很有前途的途径。远程随访通常基于医疗服务提供者对远程患者问卷调查结果的评估。
该研究的目的是采用德尔菲法,确定一份通过问卷评估的参数清单,以便日后应用于炎症性肠病患者的随访和治疗。
材料和方法。参与研究的专家组由具有不同工作经验的消化内科医生组成。我们制作了一份电子调查表来收集信息。在填写问卷时,必须注明参与者的工作年限。研究分为三个阶段。在第一阶段,受访者回答了一个开放式问题,即应该对炎症性肠病患者的哪些参数进行评估。在第二阶段,受访者回答了同样的问题。但在这一阶段,他们从建议的项目中选择项目,项目数量不限。研究的第三阶段是对回答进行分析。每个参数的主要终点是75%以上的受访者达成共识。
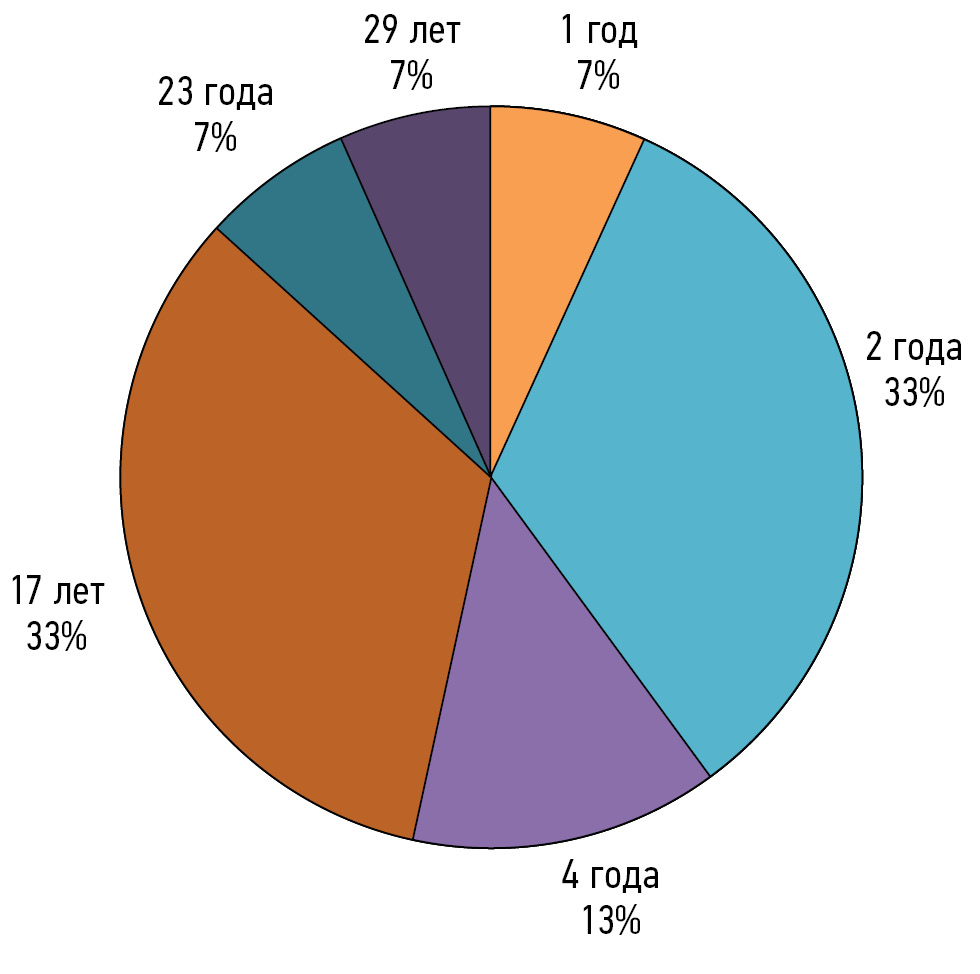
结果。15人参与了研究,其中13.3%为男性。在所有受访者中,46%在门诊机构工作,54%在医院工作。年龄范围为25岁至53岁之间。同时,53%的参与者拥有1至4年的工作经验,47%的参与者拥有17至29年的工作经验。在第一阶段结束时,没有一个参数达到75%的同意程度。第二阶段结束后,受访者对72%的参数达成了一致意见。在第一阶段和第二阶段,受访者的年龄、性别、工作年限和工作地点与答复之间都未发现相关性。
结论。炎症性肠病患者治疗和随访期间的最终评估参数清单包括:腹痛;排便次数和粪便质量;粪便中是否有病理性杂质;体温;关节/肌肉疼痛;睡眠质量;情绪状态:焦虑、情绪;工作的人的工作能力/学习的人的上课能力;精力、体力;对疾病的固执;患者对其生活质量的总体评价;坚持治疗的情况。
作者简介
Yuliya F. Shumskaya
Research and Practical Clinical Center for Diagnostics and Telemedicine Technologies
编辑信件的主要联系方式.
Email: shumskayayf@zdrav.mos.ru
ORCID iD: 0000-0002-8521-4045
SPIN 代码: 3164-5518
俄罗斯联邦, Moscow
Dina A. Akhmedzyanova
Research and Practical Clinical Center for Diagnostics and Telemedicine Technologies
Email: AkhmedzyanovaDA@zdrav.mos.ru
ORCID iD: 0000-0001-7705-9754
SPIN 代码: 6983-5991
俄罗斯联邦, Moscow
Marina G. Mnatsakanyan
The First Sechenov Moscow State Medical University
Email: mnatsakanyan_m_g@staff.sechenov.ru
ORCID iD: 0000-0001-9337-7453
SPIN 代码: 2015-1822
MD, Dr. Sci. (Med.), Professor
俄罗斯联邦, MoscowKsenia Y. Kolosova
The First Sechenov Moscow State Medical University
Email: kolosova_k_yu@staff.sechenov.ru
ORCID iD: 0000-0001-7641-2755
MD, Cand. Sci. (Med.)
俄罗斯联邦, MoscowOlga V. Tashchyаn
The First Sechenov Moscow State Medical University
Email: olgatash1@rambler.ru
ORCID iD: 0000-0001-6759-6820
MD, Cand. Sci. (Med.)
俄罗斯联邦, MoscowMarta V. Yurazh
The First Sechenov Moscow State Medical University
Email: yurazh_m_v@staff.sechenov.ru
ORCID iD: 0000-0002-4459-7481
SPIN 代码: 4872-7130
俄罗斯联邦, Moscow
Roman V. Reshetnikov
Research and Practical Clinical Center for Diagnostics and Telemedicine Technologies
Email: reshetnikov@fbb.msu.ru
ORCID iD: 0000-0002-9661-0254
SPIN 代码: 8592-0558
Cand. Sci. (Phys.-Math.)
俄罗斯联邦, Moscow参考
- Romberg-Camps MJL, Bol Y, Dagnelie PC, et al. Fatigue and health-related quality of life in inflammatory bowel disease. Inflammatory Bowel Diseases. 2010;16(12):2137–2147. doi: 10.1002/ibd.21285
- Windsor JW, Kaplan GG. Evolving Epidemiology of IBD. Current Gastroenterology Reports. 2019;21(8. doi: 10.1007/s11894-019-0705-6
- Khalif IL, Shapina MV. Inflammatory bowel disease treatment in Eastern Europe. Current Opinion in Gastroenterology. 2017;33(4):230–233. doi: 10.1097/mog.0000000000000370
- Belousova EA, Shelygin YuA, Achkasov SI, et al. Clinical and Demographic Features and Treatment Approaches for Inflammatory Bowel Diseases (Crohn’s Disease, Ulcerative Colitis) in the Russia. The Primery Results of the Analysis of the National Register. Koloproktologia. 2023;22(1):65–82. (In Russ) doi: 10.33878/2073-7556-2023-22-1-65-82
- Pang L, Liu H, Liu Zh, et al. Role of Telemedicine in Inflammatory Bowel Disease: Systematic Review and Meta-analysis of Randomized Controlled Trials. Journal of Medical Internet Research. 2022;24(3):e28978. doi: 10.2196/28978
- Trieschmann K, Chang L, Park S, et al. The visceral sensitivity index: A novel tool for measuring GI-symptom-specific anxiety in inflammatory bowel disease. Neurogastroenterology & Motility. 2022;34(9). doi: 10.1111/nmo.14384
- Jackson BD, Con D, Gorelik A, et al. Examination of the relationship between disease activity and patient-reported outcome measures in an inflammatory bowel disease cohort. Internal Medicine Journal. 2018;48(10):1234–1241. doi: 10.1111/imj.13937
- Thomas PWA, Broeder N, Derikx M, et al. Impact of Biological Therapies and Tofacitinib on Real-world Work Impairment in Inflammatory Bowel Disease Patients: A Prospective Study. Inflammatory Bowel Diseases. 2022;28(12):1813–1820. doi: 10.1093/ibd/izac002
- Chen B, Zhou B, Song G, et al. Inflammatory bowel disease is associated with worse sexual function: a systematic review and meta-analysis. Translational Andrology and Urology. 2022;11(7):959–973. doi: 10.21037/tau-22-190
- Murphy MK, Black NA, Lamping DL, et al. Consensus development methods, and their use in clinical guideline development. Health Technology Assessment. 1998;2(3):I–IV. doi: 10.3310/hta2030
- Williams PL, Webb C. The Delphi technique: a methodological discussion. Journal of Advanced Nursing. 1994;19(1):180–186. doi: 10.1111/j.1365-2648.1994.tb01066.x
- Wilhelm W. Alchemy of the Oracle: the Delphi technique. The Delta Pi Epsilon Journal. 2001;43:6–26.
- Akins RB, Tolson H, Cole BR. Stability of response characteristics of a Delphi panel: application of bootstrap data expansion. BMC Medical Research Methodology. 2005;5(1). doi: 10.1186/1471-2288-5-37
- Diamond IR, Grant RC, Feldman BM, et al. Defining consensus: A systematic review recommends methodologic criteria for reporting of Delphi studies. Journal of Clinical Epidemiology. 2014;67(4):401–409. doi: 10.1016/j.jclinepi.2013.12.002
- Andel EM, Koopmann BDM, Crouwel F, et al. Systematic Review of Development and Content Validity of Patient-reported Outcome Measures in Inflammatory Bowel Disease: Do We Measure What We Measure? Journal of Crohn’s and Colitis. 2020;14(9):1299–1315. doi: 10.1093/ecco-jcc/jjaa057
- Barberio B, Zamani M, Black CJ, et al. Prevalence of symptoms of anxiety and depression in patients with inflammatory bowel disease: a systematic review and meta-analysis. The Lancet Gastroenterology & Hepatology. 2021;6(5):359–370. doi: 10.1016/s2468-1253(21)00014-5
- Halpin SJ, Ford AC. Prevalence of Symptoms Meeting Criteria for Irritable Bowel Syndrome in Inflammatory Bowel Disease: Systematic Review and Meta-Analysis. American Journal of Gastroenterology. 2012;107(10):1474–1482. doi: 10.1038/ajg.2012.260
- Yu N, Basnayake C, Connell W, et al. Interventions to Improve Adherence to Preventive Care in Inflammatory Bowel Disease: A Systematic Review. Inflammatory Bowel Diseases. 2022;28(8):1177–1188. doi: 10.1093/ibd/izab247
- Vinogradova IA, Nizovtsova LA, Omelyanskaya OV. Innovative strategic session in the scientific activity of the Center for Diagnostics and Telemedicine. Digital Diagnostics. 2023;3(4):414–420. (In Russ) doi: 10.17816/DD111833
补充文件