当对孕妇进行电子计算机断层扫描时胎儿吸收剂量的评估:系统综述
- 作者: Vodovatov A.V.1, Golchenko O.A.2, Mashchenko I.A.3, Alekseeva D.V.3, Chipiga L.A.1,3, Khutornoy I.V.4, Kozlova P.V.3, Trufanov G.E.3, Druzhinina P.S.1, Ryzhov S.A.5, Soldatov I.V.5
-
隶属关系:
- Saint-Petersburg Research Institute of Radiation Hygiene after Professor P.V. Ramzaev
- City polyclinic № 19
- Almazov National Medical Research Centre
- Lomonosov Moscow State University
- Research and Practice Center of Diagnostics and Telemedicine Technologies
- 期: 卷 4, 编号 2 (2023)
- 页面: 170-184
- 栏目: 系统评价
- URL: https://journals.rcsi.science/DD/article/view/146884
- DOI: https://doi.org/10.17816/DD472150
- ID: 146884
如何引用文章
详细
论证。由于在国内实践中缺乏经批准的计算方法和关于当对孕妇进行X线放射检查时胎儿辐射剂量的系统化数据,因此在实践中很难应用这些检查方法。该问题对于电子计算机断层扫描来说尤其重要,因为虽然该这个问题对于电子计算机断层扫描是一种被广泛使用的、信息量大的放射诊断技术,但是与较高病人辐射剂量有关的。
该研究的目的是使现有的关于进行电子计算机断层扫描时胎儿吸收剂量的数据系统化。
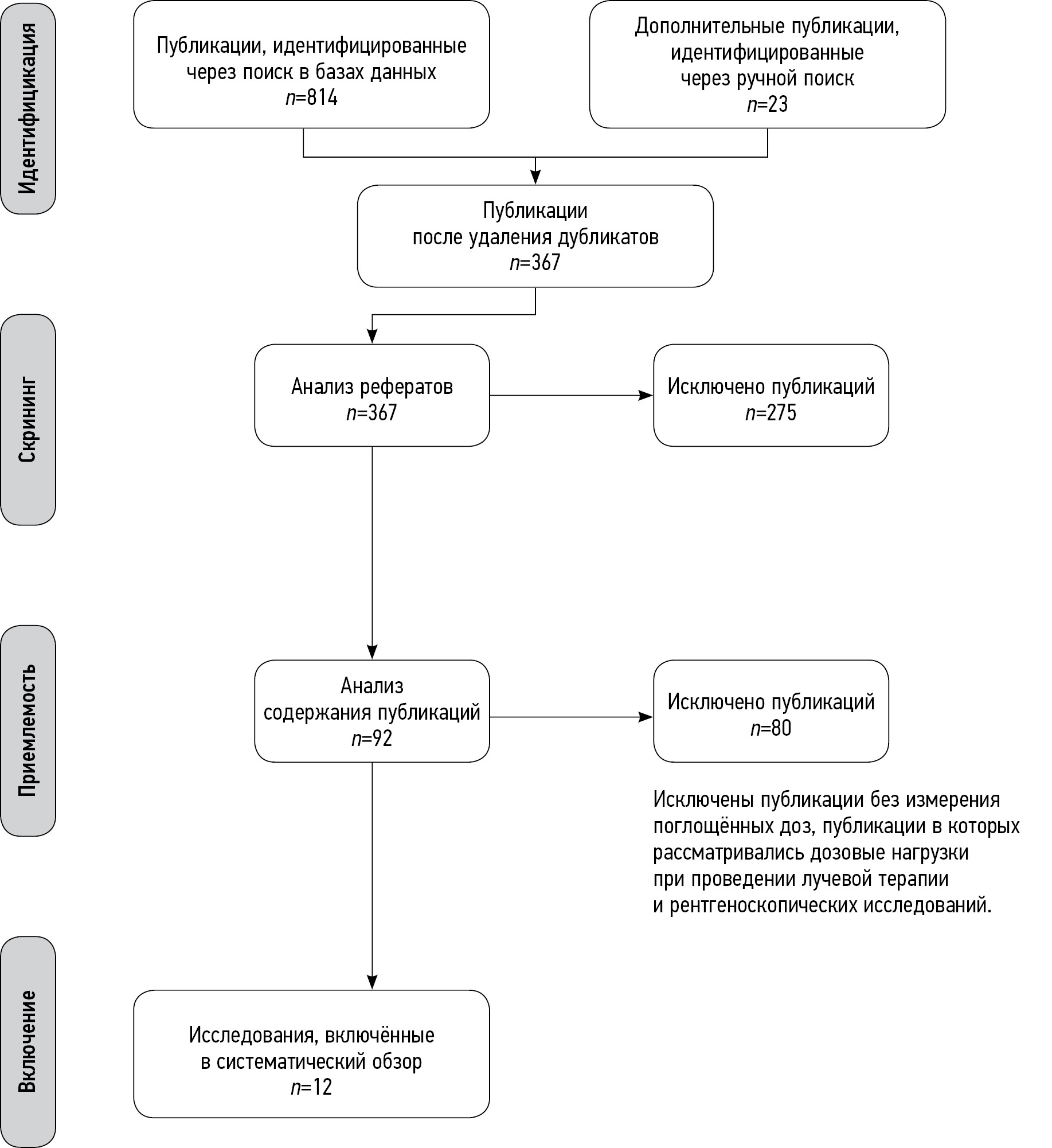
材料和方法。对俄文和英文出版物进行了搜索和分析。在PubMed/Medline、Google Scholar和eLibrary系统中进行了搜索。最后的分析包括12份出版物,其中有8项使用拟人模型的研究、3项回顾性研究和1个前瞻性临床研究。
结果。当进行腹部、盆腔和全身电子计算机断层扫描时胎儿吸收的剂量最高。在审查所包括的出版物中,没有关于超过胎儿剂量限制的报告。
结论。无论扫描区域如何,对孕妇进行一次性单相电子计算机断层扫描的时候,超过胎儿吸收剂量限制(100 mGy)是不太可能的,因此,有需要的话,可以对孕妇进行这样的检查。然而,在进行腹部、盆腔或受伤全身的多次或多相电子计算机断层扫描的情况下,会超过这个阈值。在这种情况下,多科目辐射安全小组(放射科医生和临床专家)应该进行额外的风险评估。
作者简介
Aleksandr V. Vodovatov
Saint-Petersburg Research Institute of Radiation Hygiene after Professor P.V. Ramzaev
Email: vodovatoff@gmail.com
ORCID iD: 0000-0002-5191-7535
SPIN 代码: 4560-8978
Cand. Sci. (Biol.)
俄罗斯联邦, Saint PetersburgOlga A. Golchenko
City polyclinic № 19
Email: breakerxolyga@yandex.ru
ORCID iD: 0000-0003-4614-9241
俄罗斯联邦, Saint Petersburg
Irina A. Mashchenko
Almazov National Medical Research Centre
Email: mashchenko_ia@almazovcentre.ru
ORCID iD: 0000-0002-4949-8829
SPIN 代码: 5154-7080
MD, Cand. Sci. (Med.), Leading Researcher, Assistant Professor
俄罗斯联邦, Saint PetersburgDarya V. Alekseeva
Almazov National Medical Research Centre
Email: darja-karpova@yandex.ru
ORCID iD: 0000-0001-9528-9377
SPIN 代码: 6484-4327
Assistant Lecturer
俄罗斯联邦, Saint PetersburgLarisa A. Chipiga
Saint-Petersburg Research Institute of Radiation Hygiene after Professor P.V. Ramzaev; Almazov National Medical Research Centre
Email: larisa.chipiga@gmail.com
ORCID iD: 0000-0001-9153-3061
SPIN 代码: 3920-7798
Cand. Sci. (Engin.), Research Associate, Assistant Professor
俄罗斯联邦, Saint Petersburg; Saint PetersburgIvan V. Khutornoy
Lomonosov Moscow State University
Email: mcdm.avk@gmail.com
ORCID iD: 0000-0002-5405-603X
SPIN 代码: 8020-0222
Graduate Student
俄罗斯联邦, MoscowPolina V. Kozlova
Almazov National Medical Research Centre
Email: apollinaria@bk.ru
ORCID iD: 0000-0002-3240-7038
SPIN 代码: 3555-0410
Assistant Lecturer
俄罗斯联邦, Saint PetersburgGennady E. Trufanov
Almazov National Medical Research Centre
Email: trufanovge@mail.ru
ORCID iD: 0000-0002-1611-5000
SPIN 代码: 3139-3581
MD, Dr. Sci. (Med.)
俄罗斯联邦, Saint PetersburgPolina S. Druzhinina
Saint-Petersburg Research Institute of Radiation Hygiene after Professor P.V. Ramzaev
Email: druzhininapauline@gmail.com
ORCID iD: 0000-0003-2921-067X
SPIN 代码: 9003-3234
Junior Research Associate
俄罗斯联邦, Saint PetersburgSergey A. Ryzhov
Research and Practice Center of Diagnostics and Telemedicine Technologies
Email: mosrg@mail.ru
ORCID iD: 0000-0002-0640-7368
SPIN 代码: 6595-4011
Research Associate
俄罗斯联邦, MoscowIlia V. Soldatov
Research and Practice Center of Diagnostics and Telemedicine Technologies
编辑信件的主要联系方式.
Email: SoldatovIV2@zdrav.mos.ru
ORCID iD: 0000-0002-4867-0746
SPIN 代码: 4065-6048
俄罗斯联邦, Moscow
参考
- Shtentsel RE, Semenova ES, Mashchenko IA, et al. The history of the formation and development of methods of radiation diagnostics in perinatology. Translational Med. 2021;8(3):29–36. (In Russ). doi: 10.18705/2311-4495-2021-8-3-29-36
- Sadro C, Bernstein MP, Kanal KM. Imaging of trauma. Part 2, Abdominal trauma and pregnancy: A radiologist’s guide to doing what is best for the mother and baby. Am J Roentgenol. 2012;199(6):1207–1219. doi: 10.2214/AJR.12.9091
- Wang PI, Chong ST, Kielar AZ, et al. Imaging of pregnant and lactating patients: Part 1, evidence-based review and recommendations. Am J Roentgenol. 2012;198(4):778–784. doi: 10.2214/AJR.11.7405
- Committee Opinion No. 723: Guidelines for diagnostic imaging during pregnancy and lactation. Obstet Gynecol. 2017;130(4):210–216. doi: 10.1097/AOG.0000000000002355
- ICRP. Recommendations International Commission on Radiation Protection 2007. Publication ICRP No. 103. Transl. from English. Ed. by M.F. Kiselev and N.K. Shandala. Moscow: Alana; 2009. 312 р.
- ACR-SPR practice parameter for imaging pregnant or potentially pregnant adolescents and women with ionizing radiation. 2018. 23 p. Available from: https://www.acr.org/-/media/acr/files/practice-parameters/pregnant-pts.pdf. Accessed: 17.05.2023.
- Frush D. The cumulative radiation dose paradigm in pediatric imaging. Br J Radiol. 2021;94(1126):20210478. doi: 10.1259/bjr.20210478
- Vodovatov AV, Chipiga LA, Piven PA, et al. Assessment of the absorbed doses in the fetus from the computed tomography of the chest for the pregnant women. Radiatsionnaya Gygiena. 2021;14(3):126–135. (In Russ). doi: 10.21514/1998-426X-2021-14-3-126-135
- Liu H, Liu F, Li J, et al. Clinical and CT imaging features of the COVID-19 pneumonia: Focus on pregnant women and children. J Infect. 2020;80(5):7–13. doi: 10.1016/j.jinf.2020.03.007
- Dehan L, Lin L, Xin W, et al. Pregnancy and perinatal outcomes of women with coronavirus disease (COVID-19) pneumonia: A preliminary analysis. Am J Roentgenol. 2020;215(1):127–132. doi: 10.2214/AJR.20.23072
- Garcia EM, Camacho MA, Karolyi DR, et al.; Expert Panel on Gastrointestinal Imaging. ACR appropriateness criteria right lower quadrant pain-suspected appendicitis. Am J Roentgenol. 2018;15(11):373–387. doi: 10.1016/j.jacr.2018.09.033
- Sazhin AV, Kirienko AI, Kurtser MA, et al. Acute appendicitis during pregnancy (in Russian only). Pirogov Russian Journal of Surgery. 2019;(1):70–77. (In Russ).
- Gu J, Bednarz B, Caracappa PF, Xu XG. The development, validation and application of a multi-detector CT (MDCT) scanner model for assessing organ doses to the pregnant patient and the fetus using Monte Carlo simulations. Phys Med Biol. 2009;54(9):2699–2717. doi: 10.1088/0031-9155/54/9/007
- Kelaranta A, Mäkelä T, Kaasalainen T, Kortesniemi M. Fetal radiation dose in three common CT examinations during pregnancy: Monte Carlo study. Phys Med. 2017;(43):199–206. doi: 10.1016/j.ejmp.2017.09.120
- Angel E, Wellnitz CV, Goodsitt MM, et al. Radiation dose to the fetus for pregnant patients undergoing multidetector CT imaging: Monte Carlo simulations estimating fetal dose for a range of gestational age and patient size. Radiology. 2008;249(1):220–227. doi: 10.1148/radiol.2491071665
- Goldberg-Stein S, Liu B, Hahn PF, Lee SI. Body CT during pregnancy: Utilization trends, examination indications, and fetal radiation doses. Am J Roentgenol. 2011;196(1):146–151. doi: 10.2214/AJR.10.4271
- Vandecaveye V, Amant F, Lecouvet F, et al. Imaging modalities in pregnant cancer patients. Int J Gynecol Cancer. 2021;31(3):423–431. doi: 10.1136/ijgc-2020-001779
- Kwan ML, Miglioretti DL, Marlow EC, et al.; Radiation-Induced Cancers Study Team. Trends in medical imaging during pregnancy in the United States and Ontario, Canada, 1996 to 2016. JAMA Network Open. 2019(7):197–249. doi: 10.1001/jamanetworkopen.2019.7249
- Prokop M, Galanski M. Spiral and multilayered computed tomography. Moscow; 2011. 440 р. (In Russ).
- Arablinskiy AV, Magdebura YA. CT in the diagnosis of nontraumatic acute abdomen. REJR. 2018;8(2):58–71. (In Russ). doi: 10.21569/2222-7415-2018-8-2-58-71
- Kirsch J, Brown RK, Henry TS, et al.; Expert Panels on Cardiac and Thoracic Imaging. ACR appropriateness criteria acute chest pain-suspected pulmonary embolism. J Am Coll Radiol. 2017;14(5):2–12. doi: 10.1016/j.jacr.2017.02.027
- Shyu JY, Khurana B, Soto JA, et al. Expert Panel on Major Trauma Imaging. ACR appropriateness criteria major blunt trauma. J Am Coll Radiol. 2020;17(5):160–174. doi: 10.1016/j.jacr.2020.01.024
- Panchenko EP, Balahonova TV, Danilov NM, et al. Diagnosis and management of pulmonary embolism Eurasian Association of Cardiology (EAC) clinical practice guidelines (2021). Eurasian Heart J. 2021;(1):44–77. (In Russ). doi: 10.381092225-1685-2021-1-44-77
- Ria F, D’Ercole L, Origgi D, et al.; Association of Medical Physics Task Group. Statement of the Italian Association of Medical Physics (AIFM) task group on radiation dose monitoring systems. Insights Imaging. 2022;13(1):23. doi: 10.1186/s13244-022-01155-1
- Sensakovic WF, Royall I, Hough M, et al. Fetal dosimetry at CT: A primer. Radiographics. 2020;40(4):1061–1070. doi: 10.1148/rg.2020190166
- Jaffe TA, Yoshizumi TT, Toncheva GI, et al. Early first-trimester fetal radiation dose estimation in 16-MDCT without and with automated tube current modulation. Am J Roentgenol. 2008;190(4):860–864. doi: 10.2214/AJR.07.2925
- Huda W, Randazzo W, Tipnis S, et al. Embryo dose estimates in body CT. Am J Roentgenol. 2010;194(4):874–880. doi: 10.2214/AJR.09.4032
- Damilakis J, Perisinakis K, Tzedakis A, et al. Radiation dose to the conceptus from multidetector CT during early gestation: A method that allows for variations in maternal body size and conceptus position. Radiology. 2010;257(2):483–489. doi: 10.1148/radiol.10092397
- Lazarus E, Debenedectis C, North D, et al. Utilization of imaging in pregnant patients: 10-year review of 5270 examinations in 3285 patients 1997–2006. Radiology. 2009;251(2):517–524. doi: 10.1148/radiol.2512080736
- Lazarus E, Mayo-Smith WW, Mainiero MB, Spencer PK. CT in the evaluation of nontraumatic abdominal pain in pregnant women. Radiology. 2007;244(3):784–790. doi: 10.1148/radiol.2443061634
- Goldberg-Stein SA, Liu B, Hahn PF, Lee SI. Radiation dose management: Part 2, estimating fetal radiation risk from CT during pregnancy. Am J Roentgenol. 2012;198(4):352–356. doi: 10.2214/AJR.11.7458
- Litmanovich D, Boiselle PM, Bankier AA, et al. Dose reduction in computed tomographic angiography of pregnant patients with suspected acute pulmonary embolism. J Comput Assist Tomogr. 2009;33(6):961–966. doi: 10.1097/RCT.0b013e318198cd18
- Begano D, Söderberg M, Bolejko A. To use or not use patient shielding on pregnant women undergoing CT pulmonary angiography: A phantom study. Radiation Protection Dosimetry. 2020;189(4):458–465.
- Ryckx N, Sans-Merce M, Schmidt S, et al. The use of out-of-plane high Z patient shielding for fetal dose reduction in computed tomography: Literature review and comparison with Monte-Carlo calculations of an alternative optimisation technique. Phys Med. 2018;(48):156–161. doi: 10.1016/j.ejmp.2018.03.017
- Tack D, Kalra MK, Gevenois PA. Radiation dose from multidetector CT (2nd ed.). Springer; 2012. doi: 10.1007/978-3-642-24535-0
- Doshi SK, Negus IS, Oduko JM. Fetal radiation dose from CT pulmonary angiography in late pregnancy: A phantom study. Br J Radiol. 2008;81(968):653–658. doi: 10.1259/bjr/22775594
- Gilet AG, Dunkin JM, Fernandez TJ, et al. Fetal radiation dose during gestation estimated on an anthropomorphic phantom for three generations of CT scanners. Am J Roentgenol. 2011;196(5):1133–1137. doi: 10.2214/AJR.10.4497
补充文件