The role of local anesthesia to reduce pain after PСNL
- Authors: Popov S.V1, Orlov I.N1, Obidnyak V.M1, Malevich S.M1, Borichev M.V1, Basok S.M1, Gadzhiev N.K2, Tagirov N.S3, Pisarev A.V4, Malkhasyan V.A5, Mazurenko D.A6
-
Affiliations:
- St Petersburg St Luka Clinical Hospital
- Nikiforov Russian Center of Emergency and Radiation Medicine
- St Petersburg St Elisabeth City Hospital
- St Petersburg Multiprofile Center, Ministry of Health of Russian Federation
- Moscow State Medical Stomatological University named after A.I. Evdokimov
- Urologic Clinic EMC
- Issue: Vol 7, No 4 (2016)
- Pages: 113-118
- Section: Articles
- URL: https://journals.rcsi.science/pediatr/article/view/5976
- DOI: https://doi.org/10.17816/PED74113-118
- ID: 5976
Cite item
Full Text
Abstract
The goal of the study was to assess the level of postoperative pain in patients undergoing PCNL after paratubal infiltration with local anesthetic to compare this method of anesthesia with a control group where local anesthesia was not provided. 63 patients were included with kidney stones, confirmed by computer tomography (CT), who were planned to undergo percutaneous nephrolithitomy (PСNL). During the observation 6 patients have been excluded in accordance with the exclusion criteria. The remaining 57 patients were randomized into 2 groups: group A (n= 28) at the end of the operation received paratubal infiltration of 0.5% sol. ropivacaine; group B (n= 29) (controls) — local anesthesia was not used. Postoperative pain was assessed by means of VAS-score 1 hour, 6 hours and 24 hours after surgery. Systemic analgesia was performed with NSAIDs (intramuscular injection of 100 mg ketoprofen) when requested by the patient (Patient-Controlled Analgesia). In patients with local anesthesia, the total VAS score evaluated after 1 and 6 hours after the operation was significantly lower than in the control group. The average amount of ketoprofen required for postoperative analgesia in the group of patients with paratubal infiltration was significantly lower than in the control group. Paratubal infiltration of local anesthetic after PCNL significantly reduced postoperative pain and tended to reduce the amount of NSAIDs to eliminate pain, which in turn may reduce the risk of complications associated with NSAID.
Keywords
Full Text
ВВЕДЕНИЕ
С момента, когда Fernstrom и Johanson впервые в 1976 г. использовали чрескожный доступ для удаления камней почек [9], перкутанная нефролитотрипсия (ПНЛТ) стала в какой-то степени легким и безопасным методом лечения крупных конкрементов верхних мочевых путей, отодвинув открытую хирургию на второй план. Инновационные открытия и совершенствование техники ПНЛТ сделали этот метод широко распространенным и доступным [5, 11].
Несмотря на высокую эффективность ПНЛТ, необходимость дренирования почки нефростомой и связанный с этим болевой синдром — обратная сторона медали чрескожной хирургии камней почек [10]. Существует немало работ, посвященных использованию различных техник местной анестезии и периферических нервных блокад для снижения послеоперационной боли. Применение местной анестезии в области чрескожного доступа может снизить уровень болевого синдрома и, соответственно, способствовать ранней мобилизации пациента [14, 8], что, собственно, и стало целью нашего исследования.
МАТЕРИАЛЫ И МЕТОДЫ
Дизайн исследования: проспективное рандомизированное исследование для оценки влияния местной анестезии на уровень болевого синдрома после ПНЛТ (рис. 1). После проведения этико-правовой экспертизы в исследование было включено 63 пациента с конкрементами почек, подтвержденными результатами компьютерной томографии (КТ), которым планировалось выполнить ПНЛТ. Шесть пациентов из исследования были исключены в соответствии со следующими критериями: множественные доступы при перкутанной нефролитотрипсии, аллергия на местные анестетики, инфекция в области введения анестетика, патологические изменения, деформирующие позвоночник, в том числе обострение заболеваний позвоночника; гипокоагуляция, невозможность наладить адекватную коммуникацию с пациентом. Оставшиеся 57 человек были рандомизированы в две группы:
- группа А (n = 28) — пациенты, которым выполнена паранефростомическая инфильтрация (ПНИ) с использованием 20 мл 0,5 % раствора ропивакаина после перкутанной нефролитотрипсии;
- группа B (n = 29) — группа контроля, после перкутанной нефролитотрипсии локальная анестезия не проводилась.
Рандомизация осуществлялась с использованием программы — генератора случайных чисел, для сокрытия использовался метод закрытых конвертов. «Ослепление» было односторонним — пациент не владел информацией, к какой группе пациентов он будет отнесен.
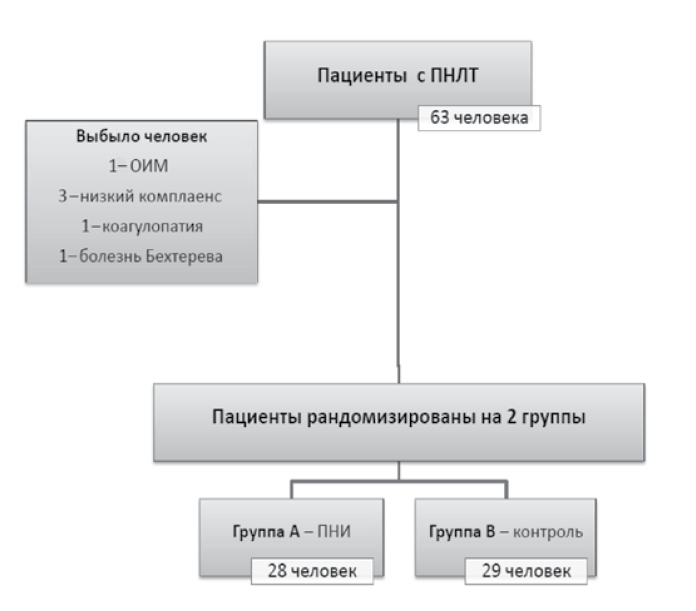
Рис. 1. Дизайн исследования: ПНЛТ — перкутанная нефролитотрипсия; ПНИ — паранефростомическая инфильтрация; ОИМ — острый инфаркт миокарда
Премедикация и анестезиологическое пособие были стандартными в обеих группах. Под общей анестезией всем пациентам устанавливался мочеточниковый катетер Ch 5. После этого с использованием литотриптора Swiss LithoClast® Master выполнялась перкутанная нефролитотрипсия в позиции пациента на животе. Всем пациентам ПНЛТ была произведена через один чрескожный доступ. Местное обезболивание выполнялось в конце операции. Техника паранефростомической инфильтрации проводилась по классической методике: под УЗ-контролем 20 мл 0,5 % раствора ропивакаина вводилось вдоль нефростомического хода от капсулы почки до кожи. При этом местное обезболивание в контрольной группе не предусматривалось.
В послеоперационном периоде болевой синдром оценивался через 1 час, 6 часов, 24 часа после операции по визуально-аналоговой шкале боли (ВАШБ). Системное обезболивание проводилось нестероидными противовоспалительными препаратами (внутримышечная инъекция 100 мг кетопрофена) по требованию пациента (Patient-Controlled Analgesia).
Статистический анализ
Рандомизация пациентов проводилась с использованием программы-генератора случайных чисел (STATISTICA 13). Статистическая достоверность полученных результатов тестировалась по значению p (p-value). При этом значения p < 0,05 расценивались как статистически достоверные. Расчеты p-value проводились с использованием медицинского софта MedCalc (версия 16.8.4).
РЕЗУЛЬТАТЫ
Демографические, интра- и периоперационные показатели представлены в табл. 1. Обе группы были гомогенными по своей структуре. В послеоперационном периоде выполнена оценка болевого синдрома по ВАШБ. Результаты представлены на рис. 2 и в табл. 2.
Таблица 1. Предоперационные показатели
Показатель | Паранефростомическая инфильтрация (n = 28) | Контроль | p-value |
Мужчины Женщины | 15 13 | 13 16 | < 0,34 < 0,46 |
Возраст, лет | 52,4 | 55,6 | < 0,98 |
Вес, кг | 84,2 | 81,4 | < 0,57 |
Рост, см | 169,8 | 172,1 | < 0,69 |
Размер камня, мм | 23,1 | 21,2 | < 0,48 |
Время операции, мин | 63,8 | 77,9 | < 0,66 |
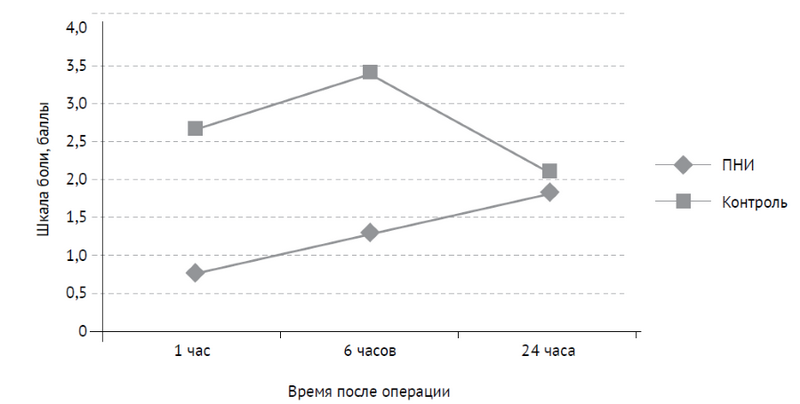
Рис. 2. Показатели шкалы боли в обеих группах после перкутанной нефролитотрипсии
Таблица 2. Показатели шкалы боли в обеих группах после перкутанной нефролитотрипсии
Показатель | Визуально-аналоговая шкала боли, средний балл | p-value | |
Паранефростомическая инфильтрация | Контроль | ||
1 час | 0,8 | 2,7 | < 0,01 |
6 часов | 1,3 | 3,4 | < 0,01 |
24 часа | 1,9 | 2,1 | > 0,05 |
В группе пациентов, которым проводилась паранефростомическая инфильтрация (ПНИ), среднее количество баллов, оцененное через 1 час и 6 часов после операции, было существенно меньше, чем в группе контроля, при этом полученные данные были статистически значимы (0,8 и 1,3 в группе ПНИ; 2,7 и 3,4 в группе контроля; p < 0,01). Через 24 часа после операции средний балл, оцененный по ВАШБ, был практически одинаковым в обеих группах (1,9 ПНИ vs 2,1 контроль; p > 0,05).
Общее количество кетопрофена, необходимого для послеоперационной анальгезии всех пациентов, в группе с ПНИ составило 1,3 г, тогда как в группе, в которой местное обезболивание не предусматривалось, — 3,1 г (p < 0,05) (табл. 3).
Таблица 3. Количество НПВС, необходимое для обезболивания всех пациентов после ПНЛТ
Количество кетопрофена, г | p-value | |
Паранефростомическая инфильтрация | Контроль | |
1,3 | 3,1 | < 0,02 |
Статистически значимой разницы в отношении длительности нефростомии и длительности госпитализации в обеих группах пациентов получено не было. Результаты представлены в табл. 4.
Таблица 4. Длительность нефростомии и госпитализации в обеих группах
Показатель | Паранефростомическая инфильтрация | Контроль | p-value |
Длительность нефростомии, дни | 2,2 | 2,4 | < 0,34 |
Длительность госпитализации, дни | 4,3 | 4,4 | < 0,56 |
ОБСУЖДЕНИЕ
За последние несколько десятилетий произошли значительные изменения в отношении методов лечения мочекаменной болезни — от открытой хирургии до минимально инвазивных эндоскопических методов лечения. В настоящее время в арсенале урологов имеется дистанционная литотрипсия, ретроградная уретеро- и нефроскопия, перкутанные методы удаления конкрементов [1]. Согласно клиническим рекомендациям камни почек более 2 см обычно подлежат удалению с использованием перкутанной нефролитотрипсии [13]. Технологический прогресс, а также совершенствование метода перкутанного доступа в полостную систему почки делает ПНЛТ относительно безопасной процедурой. ПНЛТ на сегодняшний день является «золотым стандартом» лечения крупных камней почек [2]. Обычно после перкутанной нефролитотрипсии почка дренируется нефростомическим катетером. Однако в ряде случаев возможно завершение операции без дренирования — tubeless ПНЛТ [12]. При кровотечении из паренхимы почки, длительной операции, наличии крупного или инфекционного камня установка нефростомы является обязательным этапом операции. В ряде исследований доказано, что степень послеоперационной боли прямо пропорциональна диаметру установленной нефростомы [4].
Использование мультимодальной анальгезии, то есть комбинации обезболивающих средств, которые влияют на различные процессы формирования болевого синдрома в периферической и центральной нервной системе, является неотъемлемой частью послеоперационного обезболивания [9]. Мультимодальный подход включает в себя использование системных анальгетиков (НПВС, опиоиды), местной инфильтрационной анестезии, периферических нервных блокад. Так, при выполнении межреберной блокады после ПНЛТ, по данным Honey, необходимость использования наркотических анальгетиков в послеоперационном периоде была значительно ниже [7]. K. Ak et al. использовали паравертебральную блокаду для снижения уровня послеоперационной боли и уменьшения числа случаев назначения наркотических анальгетиков [3].
Целью нашего исследования было оценить влияние паранефростомической инфильтрации на степень болевого синдрома после операции. Всем пациентам, включенным в исследование, выполнялась стандартная перкутанная нефролитотрипсия, которая заканчивалась установкой нефростомы 16/18 Ch. Было получено статистически значимое различие в уровне послеоперационной боли у пациентов в группе с обезболиванием и в группе, в которой обезболивание не предусматривалось. В группе с ПНИ уровень послеоперационной боли по ВАШБ через 1 час и 6 часов был значительно ниже, чем в группе контроля. Интересно, что через 24 часа в обеих группах уровень послеоперационной боли был практически одинаковым, что, вероятнее всего, связано с длительностью действия местного анестетика. Для 5 % раствора ропивакаина он составляет 5–12 часов [6]. Среднее количество кетопрофена, необходимого для послеоперационной анальгезии в группе с паранефростомической инфильтрацией, было существенно меньше по сравнению с группой контроля, что может влиять на риск развития гастроинтестинальных, почечных и сосудистых осложнений, связанных с применением нестероидных противовоспалительных препаратов. Значительного преимущества при использовании местной анестезии в отношении длительности госпитализации и длительности нефростомии получено не было. В нашем исследовании случаев развития аллергической реакции в ответ на инфильтрацию ткани раствором местного анестетика зарегистрировано не было.
Безусловно, исход ПНЛТ зависит от опыта хирурга. В нашей работе все оперативные вмешательства были выполнены урологами, достигшими плато в кривой обучения этого метода.
ВЫВОДЫ
Результаты данного исследования говорят о том, что использование паранефростомической инфильтрации раствором местного анестетика после ПНЛТ статистически значимо снижает уровень послеоперационной боли и позволяет уменьшить использование НПВС для устранения болевого синдрома, что, в свою очередь, может снизить риск развития осложнений, связанных с приемом НПВС. Независимо от того, какой метод используется в качестве первичной анальгезии при ПНЛТ, применение местной анестезии остается безопасным и весьма эффективным методом.
About the authors
Sergei V Popov
St Petersburg St Luka Clinical Hospital
Author for correspondence.
Email: doc.popov@gmail.com
MD, PhD, Dr. Med. Sci., Head Doctor Russian Federation
Igor N Orlov
St Petersburg St Luka Clinical Hospital
Email: doc.orlov@gmail.com
urologist, MD, PhD. Director of urologic department Russian Federation
Vladimir M Obidnyak
St Petersburg St Luka Clinical Hospital
Email: v.obidniak@gmail.com
MD, urologist. Department of Urology Russian Federation
Sergey M Malevich
St Petersburg St Luka Clinical Hospital
Email: malevichsm@gmail.com
MD, urologist. Department of Urology Russian Federation
Maxim V Borichev
St Petersburg St Luka Clinical Hospital
Email: medmaxx3@bk.ru
MD, urologist. Department of Urology Russian Federation
Stanislav M Basok
St Petersburg St Luka Clinical Hospital
Email: stas_basok@mail.ru
MD, urologist. Department of Urology Russian Federation
Nariman K Gadzhiev
Nikiforov Russian Center of Emergency and Radiation Medicine
Email: nariman.gadjiev@gmail.com
urologist, MD, PhD. Department of Urology Russian Federation
Nair S Tagirov
St Petersburg St Elisabeth City Hospital
Email: ruslana73nair@mail.ru
MD, PhD, urologist Russian Federation
Alexey V Pisarev
St Petersburg Multiprofile Center, Ministry of Health of Russian Federation
Email: alexey.v.pisarev@gmail.com
MD, urologist, Department of Urology Russian Federation
Vigen A Malkhasyan
Moscow State Medical Stomatological University named after A.I. Evdokimov
Email: vigenmalkhasyan@gmail.com
urologist, MD, PhD. Department of Urology Russian Federation
Denis A Mazurenko
Urologic Clinic EMC
Email: d.a.mazurenko@gmail.com
urologist, MD, PhD. Vice Director of Urologic Clinic Russian Federation
References
- Григорьев Н.А., Семенякин И.В., Гаджиев Н.К., и др. Мочекаменная болезнь // Урология. – 2016. – № 52. – С. 37–69. [Grigorev NA, Semenyakin IV, Gadzhiev NK, et al. Mochekamennaya bolezn. Urologiya. 2016;(52):37-69. (In Russ.)]
- Хасигов А.В., Белоусов И.И., Коган М.И. Сравнительный анализ эффективности и безопасности нефролитотомии при коралловидных камнях // Урология. – 2013. – № 1. – С. 86–88. [Hasigov AV, Belousov II, Kogan MI. Comparative assessment of percutaneous nephrolitotomia effectiveness in case of corral-like stones. Urologiya. 2013;(1):86-88. (In Russ.)]
- Ak K, et al. Thoracic paravertebral block for postoperative pain management in percutaneous nephrolithotomy patients: a randomized controlled clinical trial. Medical principles and practice. International Journal of the Kuwait University, Health Science Centre. 2013;22(3):229-33.
- Desai Mahesh R, et al. A prospective randomized comparison of type of nephrostomy drainage following percutaneous nephrostolithotomy: large bore versus small bore versus tubeless. The Journal of Urology. 2004;172(2):565-67. doi: 10.1097/01.ju.0000130752.97414.c8.
- Fernström I, Johansson B. Percutaneous Pyelolithotomy. A new extraction technique. Scandinavian Journal of Urology and Nephrology. 1976;10(3):257-59.
- Gadsen J. Local anesthetics for peripheral nerve block. The New York School of Regional Anesthesia. 2013.
- Honey R, et al. A randomized, double-blinded, placebo-controlled trial of intercostal nerve block after percutaneous nephrolithotomy. Journal of Endourology. 2013;27(4):415-19. doi: 10.1089/end.2012.0418.
- Jonnavithula Nirmala, et al. Efficacy of Peritubal Local Anesthetic Infiltration in Alleviating postoperative pain in percutaneous nephrolithotomy. Journal of Endourology. Endourological Society. 2009;23(5):857-60. doi: 10.1089/end.2008.0634.
- Joshi Girish P. Multimodal analgesia techniques and postoperative rehabilitation. Anesthesiology Clinics of North America. 2005:23(1):185-202. doi: 10.1016/j.atc.2004.11.010.
- Kim Samuel C, William W. Tinmouth, Ramsay L. Kuo. Using and choosing a nephrostomy tube after percutaneous nephrolithotomy for large or complex stone disease: a treatment strategy. Journal of Endourology. Endourological Society. 2005;19(3):348-52. doi: 10.1089/end.2005.19.348.
- Patel Sutchin R, Stephen Y. Nakada. The modern history and evolution of percutaneous nephrolithotomy. Journal of Endourology. Endourological Society. 2015;29(2):153-57. doi: 10.1089/end.2014.0287.
- Shen Pengfei, Yong Liu, Jia Wang. Nephrostomy tube-free versus nephrostomy tube for renal drainage after percutaneous nephrolithotomy: a systematic review and meta-analysis. Urologia Internationalis. 2012;88(3):298-306. doi: 10.1159/000332151.
- Türk Christian, et al. EAU guidelines on interventional treatment for urolithiasis. European Urology. 2016;69(3):475-82. doi: 10.1016/j.eururo.2015.07.041.
- Ugras Murat Yahya, Huseyin Ilksen Toprak, Hakan Gunen, et al. Instillation of skin, nephrostomy tract, and renal puncture site with ropivacaine decreases pain and improves ventilatory function after percutaneous nephrolithotomy. Journal of Endourology. Endourological Society. 2007;21(5):499-503. doi: 10.1089/end.2006.0335.
Supplementary files







